
While 60% of people over 65 report persistent pain, it doesn’t have to be an inevitable part of aging.
This graph offers an interesting perspective and is worth a closer look. The green line shows that age-related changes in the spine increase over time, while the blue line indicates that people seek the most medical care for back pain in their 40s and 50s.
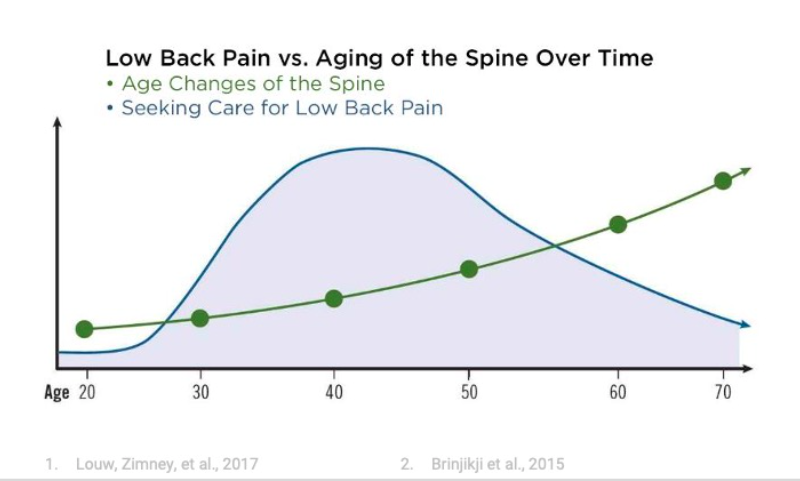
The graph reveals an interesting pattern: although spinal changes increase with age, the highest rates of medical visits for back pain occur in midlife. Notably, a 2015 study published in the Journal of Neuroradiology (referenced in the figure above) found that many participants with degenerative changes on imaging reported no pain. This suggests that many of these changes are likely a normal part of aging and not necessarily linked to symptoms.
Pain, Fear, and the Brain
Pain is the body’s natural alarm system, alerting us to injury or disease. Ideally, as healing occurs, the alarm subsides. However, in 1 out of 4 people, this alarm stays activated even after the tissues have healed.
This means pain doesn’t always equal tissue damage—it can persist due to changes in the nervous system.
Fear and inactivity can also contribute to pain. When people avoid movement out of fear, their brain can actually amplify pain signals. Unfortunately, medical professionals sometimes use fear-inducing language—saying things like, “You have the back of a 90-year-old” or “Your knee is bone-on-bone.” This messaging can make patients more anxious about movement, reinforcing pain through a process called catastrophizing.
Pain scientist and physical therapist Adriaan Louw describes catastrophizing as persistently expecting the worst—like seeing the glass not just half empty, but completely shattered. When the brain goes on fear alert the happy chemicals in the brain dry up and pain is amplified.
The good news? Research consistently shows that when people understand what’s causing their pain, their perception of it decreases. Knowledge is power—and movement is key to breaking the pain-fear cycle.
Pain and Inactivity
Our bodies are designed for movement. Many older adults experience pain not because of aging, but because they aren’t moving enough.

Movement Lubricates Joints
As Adriaan Louw says, “Motion is lotion.” Movement stimulates the production of synovial fluid, which helps joints glide smoothly and reduces stiffness.
Movement Improves Circulation
Increased blood flow delivers oxygen and nutrients to tissues while flushing out inflammatory byproducts that contribute to pain. This is the reason some people feel more pain at night. Our blood pressure decreases as we sleep so our nerves get less oxygen and nutrient rich blood.
Movement Releases Endorphins
Physical activity triggers the release of natural painkillers (endorphins), which improve mood and reduce discomfort. (For more information about the happy chemicals, see our blog: Unlock Happiness With The Happy Hormones .)
Movement Reduces Sensitization
Chronic pain can lead to an overactive nervous system, making the brain less precise in identifying the source of discomfort. When we stop moving a painful body part, the brain’s “map” of that area becomes blurry, which can actually increase pain sensitivity.
For example, if you injure your shoulder, you might avoid moving it due to pain and fear of worsening the injury. Over time, this lack of movement can cause the brain to perceive pain in a larger area, making your whole arm feel sore.
Similarly, if someone wears stiff orthopedic shoes that restrict foot movement, the brain receives less sensory input from the feet. Over time, this can contribute to discomfort and pain, even beyond the original issue.
The good news? Gradual, gentle movement helps retrain the nervous system, sharpen the body’s map, and reduce pain over time. Keeping the body in motion is key to breaking the cycle of sensitization and discomfort.
Don’t Let Pain Stop You from Moving
Sharp, sudden pain during exercise is a red flag, but mild, ongoing discomfort shouldn’t keep you from staying active. Avoiding movement can lead to stiffness and worsening pain, especially with conditions like arthritis. Instead, start with exercises that stay within your comfort zone and gradually build up intensity. Slowly increasing resistance and repetitions can help expand your pain tolerance over time. Consistency is key—regular movement can help your body adapt and reduce discomfort in the long run.
Pain shouldn’t be a barrier to movement—it’s often a sign that you need to move more. Start small, listen to your body, and build up gradually. Over time, movement can help retrain your nervous system, improve mobility, and reduce discomfort. Keep going—your body was made to move.
Ready to get moving again—safely and confidently?

Whether you’re dealing with chronic pain, recovering from an injury, or simply feeling stuck, our expert team is here to help. We offer personalized Physical Therapy, Occupational Therapy, and Speech Therapy assessments, all from the comfort of your home.
Serving the San Francisco Bay Area—including Santa Clara, San Mateo, San Francisco, and Marin Counties—we bring compassionate, evidence-based care right to your doorstep.
Let’s work together to keep your body in motion and your mind at ease. Contact us today to get started!
Be Active Be Well
RESOURCES
- Why You Hurt – Adriaan Louw
- Strength training may be the key to longevity. How to do it safely as you age. – LA Times
- Other books on pain by Adriaan Louw are available through OPTP
- The Way Out: A Revolutionary, Scientifically Proven Approach to Healing Chronic Pain, By Alan Gordon, LCSW
- Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations – American Journal of Neuroradiology 2015
Joanne Bedwell, PT, is the Resident Blogger at Be Active Be Well. Based in San Francisco, she lives with her husband and two nearly grown daughters. With over 25 years of experience as a physical therapist, she provides in-home client care and teaches fitness classes both in person and online.
DISCLAIMER: This article contains information that is intended to help the readers be better informed regarding exercise and health care. It is presented as general advice on health care and is not intended to be a substitute for the medical advice of a licensed physician. Before beginning any new exercise program it is recommended that you seek medical advice from your personal physician. The reader should consult with their doctor in any matters relating to his/her health.



