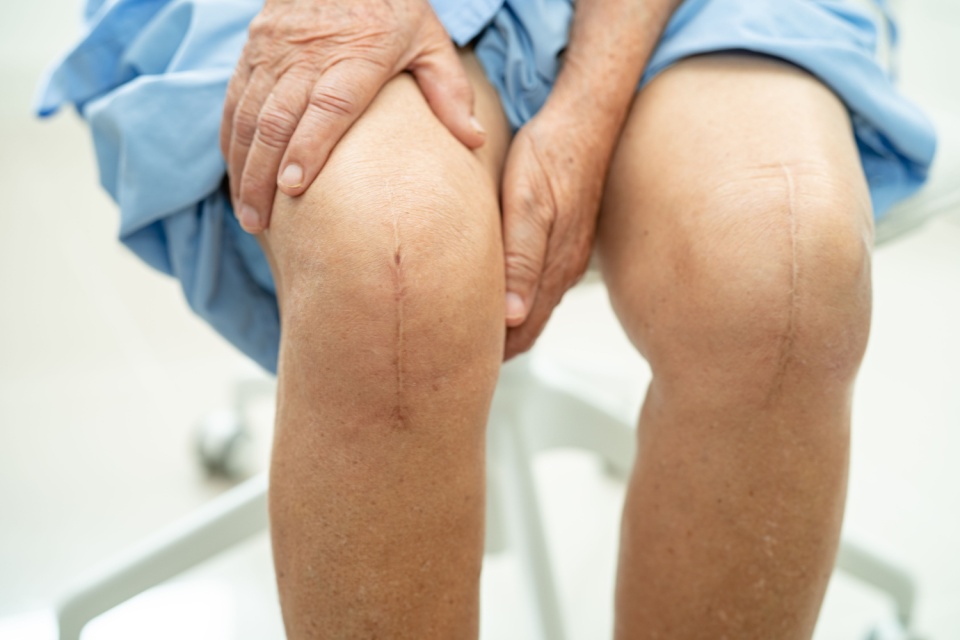
Every year, between 850,000 and 1 million people undergo knee replacement surgery. This number is expected to grow to at least 1.2 million by 2040. As a home physical therapist, I have seen countless post-op total knee replacement patients. I find that most of these patients are not prepared for what to expect after surgery. My secret suspicion is that surgeons fear if they fully described the first few weeks after surgery, no one would choose to go through with it!
Yes, your knee pain will go away and you will be able to resume your favorite activities after surgery… eventually.
Is it time to get a Total Knee Replacement?
A total knee replacement, also known as total knee arthroplasty, is often the treatment of last resort for knee pain caused by osteoarthritis. I am often asked by clients if it is “time”; should they finally get the knee replacement that the surgeon has recommended? I respond with a question: “Have you stopped doing the things in your life that give you joy because of your knee pain?” If the answer is “yes,” then it’s probably time. Additionally, by limiting your participation in activities, you are likely becoming weaker. The stronger you are going into the surgery, the better your outcome will be afterward. So don’t put it off too long.
Will the surgery take my pain away?
Yes, but it will be worse before it gets better. “THE” pain will be gone and temporarily replaced with post-surgical pain. It is important that you come to terms with this fact. A knee replacement is a major surgery, and it is normal to experience some knee pain for 6 to 9 months afterward. Bones contain many nerves, making them very sensitive when cut. This is why arthritis, which exposes the nerves in the bone as the cushioning cartilage wears away, is painful. During knee replacement surgery, the worn surfaces of the bones are removed and replaced with new, smooth surfaces. To access the bones, the surgeon also needs to cut through skin, muscle, and other soft tissues.
How can I most effectively manage the pain?
The most intense pain tends to be on day 2 or 3 after the medications and nerve blocks given during the surgery wear off. You can minimize the pain by keeping up with your pain regimen as prescribed by your surgeon. For the first week, you want to stay ahead of the pain by sticking to a schedule. Make sure to take pain medication before therapy sessions and time your range of motion exercises for 30 minutes to 1 hour after taking pain medication when it is working at its peak.
I get to lay on the sofa and rest all day for my first few weeks after surgery, right?
No! While some rest is important for healing, pain management, and decreasing swelling, regular activity is crucial for decreasing your risk of blood clots and regaining your range of motion (bending and straightening) as soon as possible.
Regaining your Knee Range of Motion Is Hard Work!
While full recovery from knee replacement surgery can take 12 to 18 months, it is crucial to regain the flexibility (bending and straightening) of your knee as soon as possible.
Within 7 to 10 days after surgery, you should aim to be able to fully straighten your knee and bend it to 90 degrees (a right angle).
Achieving this and continuing to push forward will result in excellent range of motion for your knee replacement. Recovery will require hard work and, at times, it will be painful. Post-surgical rehabilitation is demanding, and it is your responsibility to follow through. Your physical therapist can guide you, but you must do the exercises yourself.
We have therapists in the San Francisco Bay Area that can help you with both pre-surgical strengthening and post-surgical rehab at any stage.
Initially, after surgery, there is no mechanical barrier preventing you from bending or straightening your knee; pain from healing and inflamed tissues is the only obstacle. You will not damage your knee by performing your range of motion exercises; in fact, you will be aiding its recovery.
Managing swelling is crucial to this process. Reduced swelling leads to less pain, which in turn helps you regain your range of motion.
Tips To Help You Regain Your Knee Motion
Pre-medicate:
Coordinate your physical therapy and range of motion sessions with your pain medication schedule. DON’T try to do your range of motion exercises when you are due to take a dose of pain medication. DO the exercises 30 to 45 minutes after taking the medication and again well before it wears off.
Distractions:
Stretching for both knee straightening and bending will be uncomfortable. Use TV or a book as a distraction, or have a family member or friend engage you in conversation to distract you.
Knee Bending:

Sit in a chair that allows you to slide forward while keeping your feet firmly planted on the floor. Bend your knee as far as you can on your own. Then, with your feet firmly planted in place, slide forward on your chair, which will force your knee into a more bent position. Hold this position during the commercial time or for two minutes if you’re a book reader. Then relax until the next commercial or chapter break.

Place the foot of your surgical leg one step up. Holding the railing for support, rock forward and back, gradually moving deeper into knee bending.
Knee Straightening:
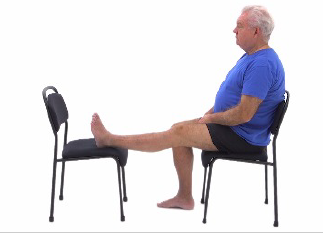
Place the heel of your surgical leg on a coffee table or stool, allowing gravity to straighten your knee. Hold for as long as you can, starting with 2 minutes and working up to 10 minutes.
Be rigorous about working on knee straightening during the day so that you can be more comfortable at night. Post-surgical instructions often tell patients that they cannot put anything under their knee for support, even when sleeping at night, for the first month. In my experience, many people have great difficulty sleeping without any knee support. If you do not get a good night’s sleep, it is that much harder to tolerate the daytime rigors of knee replacement rehab. So if you work on your knee straightening hard during the day, you can allow yourself a little comforting knee support at night.
Post-Surgical Priorities and Schedule
Initial Post-Surgical Priorities and Goals:
- Manage pain
- Decrease swelling
- Increase range of motion (bending and straightening)
- Wake up the thigh muscles
Your schedule will be something like this:
- Walk through the house
- Do your range of motion exercises
- Ice and elevate
- Repeat every 2 hours or about 5 times per day for several weeks
If you need help creating a structure for your home rehab check out our blog Making Health Habitual and Get Up and Move: How to sneak movement into your day.
Weight Bearing, Walkers, Crutches, and Canes
Unless the surgery is late in the day, you will be up and walking with a physical therapist the same day as your surgery. You will not damage your knee replacement by putting weight on that leg. On the contrary, it is important to do so. You may place as much weight onto the operated leg as your pain, comfort, common sense, and balance will allow. Your physical therapist will help you determine the correct assistive device for each stage of your rehab. For a discussion of canes vs walking poles, see our blog titled: Stride Right: Cane or Walking Poles?
Wound Care
This will vary, and you will be given instructions by your surgeon, but currently most surgeons will send you home with a dressing that does not need to be removed or changed until your follow-up office visit. Your job will be to keep it dry and the skin around the dressing clean and monitor it for any unusual signs such as excessive or unusual drainage.
Swelling
Some swelling of the knee and leg is normal after a total knee replacement, and low-level swelling may last for several months. To minimize the initial swelling, ice frequently or use an ice machine and elevate when not doing your exercises or therapy activities for the first few weeks.
Bruising
It is very common and normal for bruising of the operative leg to appear several days after surgery. You should not be alarmed. Bleeding normally occurs after a knee replacement, and this blood will track along the tissue planes of your leg, resulting in bruising of the thigh, calf, and foot/ankle. The bruising will gradually go away on its own as the body reabsorbs the blood.
Blisters
Some people will develop blisters around the knee or near the incision. There is no need to worry. They may leak some clear fluid for a period of time, but eventually, a scab will form, and they will heal.
Numbness
Most people will have an area of decreased sensation or numbness of the skin on the outer side of the knee. The nerves that provide sensation to this area of the skin need to heal and re-grow. This is normal and will resolve over 6 to 12 months.
Increased Risk of DVTs (Blood Clots)
As with any surgical procedure, there is an increased risk of developing a blood clot after knee replacement surgery. You will be given instructions and treatments from your surgeon to decrease this risk.
TED Hose/Support Hose:
Depending on your surgeon and how quickly you are sent home, you will likely be wearing support stockings initially to decrease the risk of developing a DVT (blood clot) and to decrease swelling. Your surgeon’s office will provide you with instructions on how long to wear these.
Medication – Blood Thinners:
Your surgeon may give you oral or injectable medication. It may be as simple as a daily baby aspirin. Whatever they prescribe, it is important to follow through.
Regular walking/activity:
Regular activity dramatically decreases the risk of developing a DVT. The guideline is 1-2 minutes of activity every 1-2 hours during the day. Ideally, you are getting up for a short walk at least every 2 hours. In between times, do ankle pumps.
Sleeping Problems
Most people have some difficulty sleeping for several months after a knee replacement. It will improve with time, but there are no treatments that completely solve the problem. If you feel that you are having a major problem with sleeping, discuss this with your surgeon or primary care doctor. Just know that you are not alone, and it may be a problem that you will have to work through, and time may be the only solution. Make sure you are not napping too much during the day. Even though you may not yet be able to return to your regular activities, being as active as possible during the day can help so that you are tired at bedtime.
Constipation
Due to the use of narcotic pain medications and decreased activity, constipation is common after surgery. A stool softener will be recommended as long as you are taking narcotic pain medications. In addition, make sure you stay well hydrated by drinking an adequate amount of fluids daily.
The 3 Week Slump
It is common to have a mental “slump” about 2-3 weeks after surgery. No matter how quickly they are progressing, my clients always start to question their progress. “Why am I not back to normal yet?” Remember, this is major surgery. Full recovery can take 12 to 18 months. For a time, you will have continued pain and sleep disruption. You are experiencing restrictions in your activities and a loss of autonomy. Mild, temporary depression is not uncommon.
When To Call The Surgeon
Because patients are often discharged sooner after knee replacement surgery, sometimes even on the same day, it is critical to recognize when recovery is not progressing normally and to call the surgeon’s office if necessary.

You should call your surgeon after total knee replacement surgery if you experience any of the following symptoms or concerns:
Infection:
- A fever
- Increased warmth or redness around the incision
- Drainage that is yellow in color or foul-smelling
- Red streaks leading from the incision
- A sudden increase in drainage
- Drainage lasting more than five days after your surgery
Incision:
- Gaps or breakage in the incision (if it is visible)
- Red blood saturating the dressing
Blood clot:
- Pain, swelling, or tenderness in the back of one or both lower legs: calf, back of the knee, thigh, or groin (even in your non-operated leg)
- Redness and swelling in your leg or groin
Pain:
- Severe pain not relieved by medicine, rest, or using a cold pack as directed
- New or worsening pain in your calf, ankle, or foot
Other:
- New weakness
- New numbness or tingling
- Chest pain
- Shortness of breath
Be Active Be Well
We provide in-home assessments in the San Francisco Bay Area. Contact us for a personalized Physical Therapy, Occupational Therapy, or Speech Therapy assessment.
RESOURCES
Did you find this topic interesting? Below are more in depth articles.
- I prepared for my knee replacement surgery. But I had a lot to learn. – The Washington Post
Difficulties related to the surgery are sometimes minimized by surgeons, while others say that it’s the most effective way to deal with intractable arthritis.
- Management Strategies for Orthopedic Patients – TheReadyPatient.com
Pain after surgery is a valid concern. In this article, Orthopedic Surgeon Dr. Guillaume Dumont discusses how he helps his patients.
Joanne Bedwell, PT is the Resident Blogger at Be Active Be Well. She lives and works in San Francisco with her husband and two (almost) grown daughters. Having over 25 years of experience as a physical therapist, she sees clients in their homes and teaches fitness classes in person and virtually.
DISCLAIMER: This article contains information that is intended to help the readers be better informed regarding exercise and health care. It is presented as general advice on health care. Always consult your doctor for your individual needs. Before beginning any new exercise program it is recommended that you seek medical advice from your personal physician. This article is not intended to be a substitute for the medical advice of a licensed physician. The reader should consult with their doctor in any matters relating to his/her health.



